Endometriosis
Acupuncture & Integrative Support for Endometriosis in San Diego
Endometriosis affects an estimated 1 in 10 people assigned female at birth, yet takes an average of 7 to 10 years to diagnose. It’s a chronic, inflammatory, whole-body condition where tissue similar to the uterine lining grows outside the uterus, on the ovaries, fallopian tubes, bladder, bowels, and beyond.
Endo is much more than “bad cramps.” It is a complex, full-body disease that can affect the immune system, nervous system, digestion, pelvic floor, and more. Symptoms vary widely and may include chronic pelvic pain, painful sex, bowel or bladder issues, fatigue, and infertility.
Living well with endometriosis takes a village. At Natural Harmony, acupuncture and Traditional Chinese Medicine (TCM) are central to how we approach endo, working alongside excision surgeons, pelvic floor PTs, and reproductive specialists to reduce pain, calm inflammation, and support your body’s own healing capacity.
Your symptoms are real.
You deserve to be heard.
You deserve to live well and thrive.
“I have had a wonderful experience at NHRH from the start. Everyone is incredibly thoughtful and knowledgable with infertility struggles. I was diagnosed with endometriosis about a year ago. Dr. Merritt developed a nutritional/herbal plan that focused on reducing inflammation. We had a successful IUI after working with Dr. Merritt. I love the vibe at NHRH!”


“Dr. Erin is a literal angel sent from heaven! She has helped me immensely the last few months with my endo pain. Always a pleasure to come and see her!”
Our Endometriosis Philosophy
Endo is complex, but you don’t have to navigate it alone, and you don’t have to just suffer through it. With the right tools and the right village, you can feel better, stronger, and more in control of your health.
At Natural Harmony, we believe that kind of care has to be personal. No two people experience endo the same way, and no single provider or treatment has all the answers. That’s why we show up as partners in your care, not just practitioners, helping you figure out what’s most effective and realistic for your life, every step of the way.
Our Integrative Approach to Endo
We believe combining the best of conventional and holistic medicine offers the most sustainable path to relief and vitality for people with endometriosis. For many, that means:
- Acupuncture and TCM to reduce pain, calm inflammation, regulate the cycle, and support the nervous system. Treatment is tailored to your unique presentation using acupuncture, herbal medicine, supplements, labs and lifestyle support.
- Expert excision surgery, the gold standard for removing endo tissue at its root. We work closely with SoCal’s top excision surgeons and can help you find the right fit.
- An anti-inflammatory, nutrient-dense diet to reduce the hormonal and immune drivers of endo. We’ll help you find an approach that’s sustainable, not restrictive.
- Strategic herbal and supplement protocols to support hormone metabolism, gut health, and inflammation, personalized and screened for safety alongside any treatments you’re already using.
- Gentle, pelvic-aware movement to improve circulation, reduce adhesion-related tension, and support nervous system regulation, always at a pace that works for your body.
- Functional lab testing to uncover root imbalances in hormones, gut health, immune function, and nutrient status that standard panels often miss.
- Collaboration with your care team, including your gynecologist, reproductive endocrinologist, and pelvic floor PT, to make sure every part of your plan is coordinated and working together.
This can feel like a lot to navigate. You don’t have to do everything at once, and you don’t have to do anything that doesn’t feel right for your body or your life. With the right support, endometriosis doesn’t have to define you. You can absolutely thrive.
Natural Harmony Reproductive Health specializes in caring for people with endometriosis, recognizing that many people living with this disease have traveled a long and often challenging road. Our practice is dedicated to providing a safe space to come share your story, receive support to meet your unique needs, and heal.
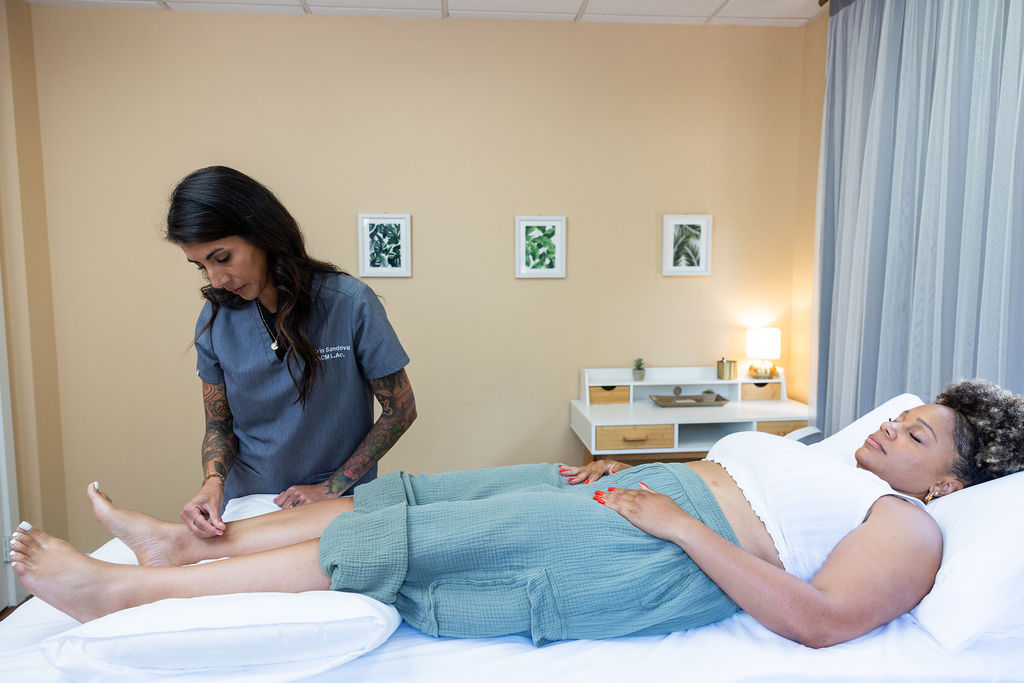
Acupuncture for Endometriosis: How It Helps
Research supports acupuncture as a meaningful integrative tool for endometriosis, with evidence for pain reduction, inflammation modulation, and improved quality of life in people with chronic pelvic conditions.
From a biomedical perspective, acupuncture works by:
- Stimulating the nervous system to release endorphins and reduce prostaglandin activity, a key driver of menstrual pain
- Modulating inflammatory cytokines, which are often elevated in endometriosis
- Improving pelvic blood flow, which supports tissue oxygenation and healing
- Regulating the hypothalamic-pituitary-ovarian (HPO) axis, helping to balance hormonal output
From a Traditional Chinese Medicine (TCM) perspective, endo is most commonly understood through the lens of qi and blood stagnation: when the smooth flow of energy and circulation through the pelvic region is impaired, pain, clotting, and tissue buildup follow. Biomedically, this maps closely to impaired pelvic microcirculation, elevated prostaglandins, and the adhesion and fibrosis characteristic of endo lesions. Other TCM patterns are frequently seen alongside endo as well, reflecting the way this disease touches so many systems at once, from immune and hormonal function to the nervous system and stress response. Your acupuncturist will identify which patterns are most active for you and build a treatment protocol around your specific presentation.
Common goals of acupuncture for endo include:
- Reducing pelvic and menstrual pain
- Improving cycle regularity and flow quality
- Calming systemic and pelvic inflammation
- Supporting immune regulation
- Reducing fatigue and improving energy
- Easing bowel and bladder symptoms
- Supporting pre- and post-surgical recovery
- Improving fertility outcomes
Many patients begin to notice meaningful shifts within 3 to 6 weeks of consistent treatment, though individual timelines vary depending on the duration and complexity of their condition.
People living with endometriosis may experience:
- Chronic, severe pain
- Inflammation
- Fatigue
- Infertility
- Extreme bloating
- Digestive issues
- Frozen pelvis
- Hormonal swings
- Severe PMS
- Pain with penetration/intercourse and more
Understanding Endometriosis - Connecting the Dots
One of the most important things to understand about endometriosis is that it’s a whole-body condition. The pain, the fatigue, the digestive issues are all connected. Endo intersects with your immune health, gut microbiome, hormonal pathways, and nervous system in ways that are deeply individual and often overlooked. The more we understand these connections, the more effectively we can support your body as a whole. Below, we break down some of the key systems involved and why they matter.
Endo + Chronic Inflammation
Endometriosis is widely recognized as an inflammatory disease. Research shows that many people with endo also experience changes in immune function. Natural killer (NK) cells, which normally help clear damaged tissue, may be less active. Other defense cells, like macrophages and T cells, don’t always work as they should.
At the same time, inflammatory signals such as cytokines and prostaglandins often run high. What’s still unclear is whether these immune shifts cause endo, or if the lesions themselves disrupt immune balance.
When inflammation persists, the body often responds by forming scar tissue. In endo, this scarring can build up over time, pulling on or blocking nearby organs. In advanced cases, it may even interfere with bowel, bladder, or reproductive function, sometimes requiring surgery to restore quality of life.
That’s why supporting immune health and reducing inflammation is such a key part of integrative endo care. By looking at a comprehensive personal history and family patterns, we can find ways to calm inflammation and help the body find a more sustainable balance.
Endo + Gut Health
Gut health is a cornerstone of endometriosis care, yet it’s often overlooked. Many people with endo know the feeling of “endo belly” – the painful bloating and discomfort that can make daily life tough. While not always, it often ties back to underlying gut imbalances.
Two patterns show up most often: dysbiosis, which is when the balance of good and bad bacteria is off (this can affect not only the gut but also the pelvis, vagina, and even the sinuses), and intestinal hyperpermeability, more commonly known as leaky gut. Research has found that people with endo may carry higher amounts of gram-negative bacteria like E. coli or Klebsiella, and some studies suggest these bacteria can even be present in the pelvic cavity itself.
Leaky gut is another key piece of the puzzle. Studies show it’s more common in those with endo, creating a cycle where a weakened gut lining drives inflammation, and inflammation worsens both gut and endo symptoms. Without support, that cycle is hard to break.
The hopeful news is that the gut can heal. When we restore balance and strengthen the gut lining, we create a healthier foundation – one that helps reduce inflammation and supports the body’s ability to better manage endometriosis.
Endo + Hormone Sensitivities
Endometriosis is considered an estrogen-sensitive disease. Even normal amounts of estrogen can fuel its growth, and a mix of genetics, environment, and lifestyle factors can all play a role. Common influences that make hormone metabolism more challenging include impaired immune or gut function, sluggish liver detox, nutrient-poor diets low in fiber, blood sugar swings, and high stress.
Estrogen isn’t the only hormone connection. Many people with endo also experience progesterone resistance, where the body’s progesterone receptors become less responsive. This resistance, often combined with chronic inflammation and estrogen dominance, may be a key reason why some patients face unexplained infertility.
Because hormone balance is just one piece of the larger endo puzzle, support needs to be comprehensive. Strategies that optimize liver detox, improve gut health, stabilize blood sugar, and strengthen nutrient intake all help create a more balanced hormonal environment – and a body that’s better able to manage endometriosis.
I must say that I went in skeptical. How can pins and needles help me with my pain? I suffer from Endometriosis and the usual aches and pains that come with getting older…
My first session with Dr. Merritt was a lot of talking about my medical background… she truly listened. It was wonderful!
Each session I go in with pain, and I walk out with none. It’s absolutely freakin’ mind-boggling!

